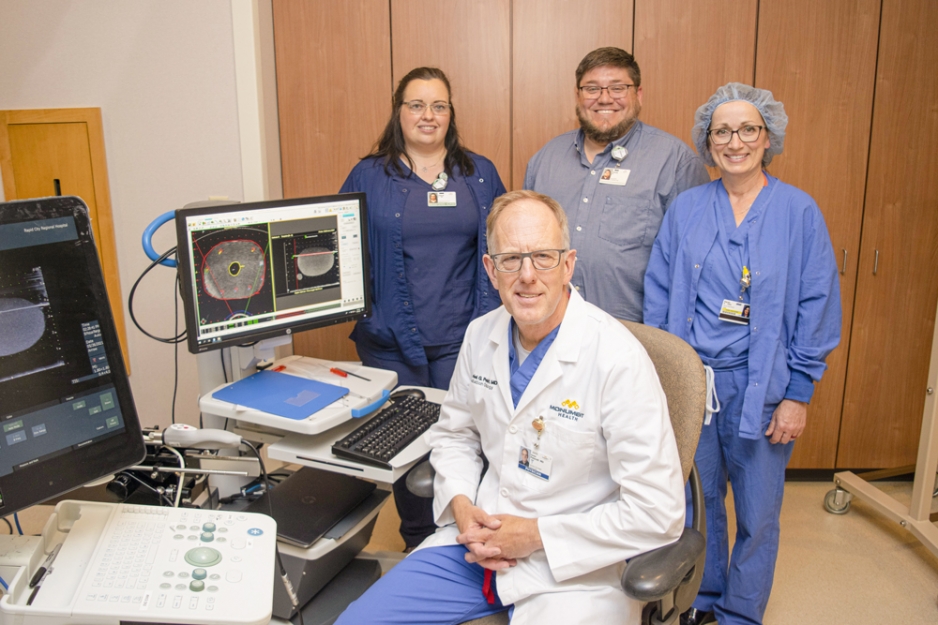
Advances in technology have allowed Daniel Petereit, M.D., Radiation Oncologist at Monument Health Cancer Care Institute, and his team to revive a type of prostate cancer treatment that was previously used in Rapid City 15 years ago.
The treatment, called high-dose-rate (HDR) brachytherapy, involves inserting a single radioactive pellet through multiple catheters into the prostate gland, delivering a highly conformal dose of radiation — which focuses the radiation in the prostate, while minimizing radiation exposure to the surrounding tissue.
With the current ultrasound-based planning system, the overall process takes about three hours and is performed on an outpatient basis. Right now, HDR brachytherapy is offered to Monument Health patients with more aggressive prostate cancer who undergo daily radiation for five weeks, followed by a brachytherapy boost to deliver a highly conformal dose.
“There is now clear evidence from randomized trials that the cure rates are 20 to 30 percent higher when using this approach compared to daily radiation alone for patients with more aggressive prostate cancers,” Dr. Petereit said. “We are now seeing more aggressive prostate cancers compared to 10 years ago when the U.S. Preventive Task Force recommended against prostate cancer screening in 2012. Fortunately, this recommendation was then reversed by the same group in 2017.”
Fifteen years ago, Dr. Petereit explained, HDR brachytherapy was performed here, but at that time it required an inpatient hospitalization, and patients were treated three to four times over two days. There is now 10 years of data that show these patients can be safely and effectively treated with a single dose of HDR brachytherapy, which allows for outpatient treatment with less patient discomfort, reduced cost and fewer urinary side effects.
The biggest advancement is the sophisticated ultrasound system that allows the oncology team to plan the accurate placement of the radioactive iridium pellet for precise treatment delivery.
Prostate Cancer
In men, the prostate is a walnut-sized gland located directly below the bladder. Prostate cancer is second only to skin cancer in cancer diagnoses for men in the United States. The American Cancer Society estimates that more than 250,000 new cases of prostate cancer will be diagnosed in the U.S. in 2022. One in eight men will be diagnosed with prostate cancer in their lifetime.
Treatment options include active surveillance, surgery, cryotherapy, hormone therapy, chemotherapy and radiation therapy – including both daily external beam radiation and brachytherapy.
Brachytherapy
Depending on the nature of the patient’s prostate cancer, brachytherapy offers one of the most favorable outcomes in terms of cure rate, patient satisfaction, cost and convenience, according to Dr. Petereit.
Unlike external beam radiation, brachytherapy involves placing the source of radiation inside the body. With low-dose-rate (LDR) brachytherapy, radioactive seeds are implanted in the prostate and left inside. The radioactivity in the seeds will decay over six months to deliver a safe, but effective dose. This approach is used for patients with less aggressive prostate cancer.
“As many of our patients live two to three hours from the Cancer Care Institute in Rapid City, this is often an ideal approach, rather than undergoing daily radiation for eight weeks,” Dr. Petereit said.
One advantage of LDR over external beam radiation is that the radiation is delivered specifically within the prostate, sparing most of the adjacent normal tissue from exposure to radiation.
Ultrasound Planning
With HDR, catheters are placed in the prostate gland to deliver a much stronger dose of radiation. The ultrasound-based planning system generates an immediate placement plan so the oncologist can optimize dose distribution. After the treatment, the catheters are removed and the patient goes home.
“My advice for patients with prostate cancer – know your options,” Dr. Petereit said. “Patients have very good options, even for high-risk disease. We see cure rates as high as 70 to 90 percent, even for more advanced prostate cancer. So, there are multiple reasons to be optimistic, even if patients present with more aggressive prostate cancer.”